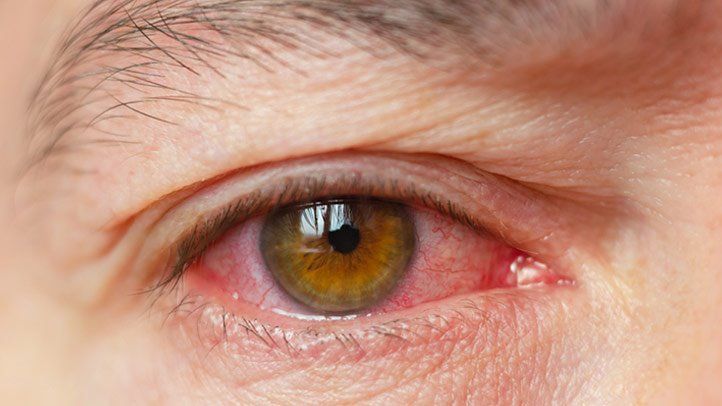
Dry Eye Syndrome, or as some people say, having dry eyes, is one of the most challenging situations for someone who has it. In dry eyes, the adequate amount of tea production is affected, and the eyes feel dry. Anyone with dry eyes would say that they have problems in continuing their daily life activities normally.
What are the causes of dry eye syndrome?
It happens because there are disturbances and balancing issues in your tear-flow system. External factors can include your AC heater or environmental change to dry out your tear film. Other causes might include:
~ Aging Process:
It is natural for people to experience dry eye, but it gets more common with age, and the older you become more prone you are to experience it. This is the result of tear production declining with old age. It usually affects people above 50, and the issue is this type of dry eye has a hard time recovering and cannot be thwarted off. Artificial tears can be used regularly to provide extra lubrication and help relieve dryness by coating your eyes.
~ Side effects of drugs/medications:
Some medications can cause mucus production some reduction and cause chronic dry eye. Medicines in this are antihistamines, diuretics, antidepressants. It is advised to talk to a Ophthalmologist in Westchester if any medication is causing you eye dryness. You can ask for an alternative or lowering the dose of drugs; if not, use artificial tears with your medication so that your eyes stay lubricated.
~ Diseases that affect your ability to make tears, like Sjogren’s syndrome:
Sjogren’s syndrome is an autoimmune condition that lets white blood cells attack your salivary glands and tear glands, thus reducing your tear production. For this, your doctor may prescribe you OTC and lubricating eye drops or a prescribed steroid eye drop. In some cases, dry eyes may not be cured by drops, and the Best eye doctor in Westchester might suggest surgery that can help preserve your tears through silicone plugs.
~ Other Autoimmune conditions:
Some other Autoimmune conditions like arthritis, lupus, and diabetes can affect your eye’s tear production. Though if you diagnose and treat the condition, it can help improve your dry eye. For an autoimmune disease, you can treat it by corticosteroid or an immunosuppressant. For diabetes, you can manage it by swearing to follow healthy lifestyle habits, diet, and medication.
~ Way too much use of electronics:
Many people who have a daily 9-hour job have 9 hours of using their laptops or pc and phones. This much amount of eyestrain or headaches caused by tension to add to this continuous screen time can lead to a dry eye. This happens because people who continuously work on laptops or computer monitors tend to blink less than they should; this leads to evaporation of moisture or tears quickly. It is recommended to blink more if you work on a computer this long because blinking can help with your eyes’ lubrication and prevent dryness and irritation. If you think that is not working correctly, you can use artificial tears while working and look about every 20 minutes and blink continuously.
What can you expect when going for a diagnosis?
There are a few tests and procedures that will determine what is causing a dry eye; they are:
~ A comprehensive eye exam: This exam includes a complete history of your eye health that can help the doctor determine the cause of dry eyes.
~ Volume of your tears will be checked: Schirmer test can be used to measure your tear production. Some blotting strips of paper are placed under your lower eyelids. After a while doctor measures the amount of tears soaked by your tears. Another option is the phenol red thread test in which the thread filled with pH-sensitive dye is placed under your lower eyelid, checked after 25 seconds of placement.
~ Osmolarity test: It checks the mixture or the composition of your tears because, with dry eye, the water is less than other materials.
~ Tear Samples: They are checked to see markers of dry eye disease, elevated matrix metalloproteinase-9, or a decreased lactoferrin.